#Epidemiology 1-A study in which researchers enrolled 52,877 women in 1990 and collected exposure and lifestyle information to assess the relationship between these factors and subsequent occurrence of cancer, is an example of which type of study? ◯ A. Cross Sectional.◯B. Prospective Cohort. ◯ C. Retrospective Cohort.
◯ D. Case-Control.
◯ E. Randomized Controlled Trial.
◯ D. Case-Control.
◯ E. Randomized Controlled Trial.
#Epidemiology 2-A 0.05 P value indicates
◯ A There is a 95% probability that the null hypothesis is correct.◯ B. There is a 95% probability that the null hypothesis is incorrect.◯ C. There is a 95% probability that the alternative hypothesis is correct.◯ D. There is a 95% probability that the alternative hypothesis is incorrect.
◯ A There is a 95% probability that the null hypothesis is correct.
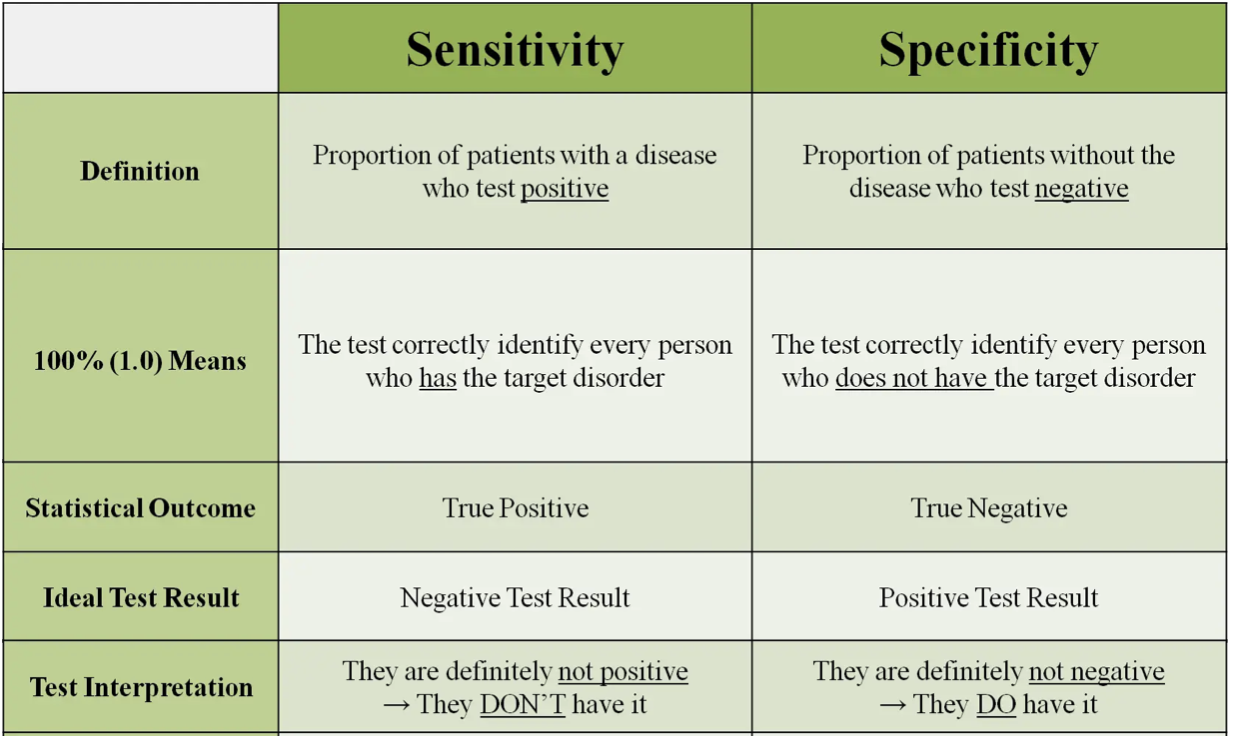
#Epidemiology 3- Test Sensitivity is defined as? ◯A. Is the ability of the test to correctly identify those without the disease.◯ B. Is the ability of a test to correctly identify those with the disease.◯ C. Is the ability of a test to correctly identify those with and without the disease.
✅ Sensitivity (75%) → How well the test detects periodontal disease.✅ Specificity (87.5%) → How well the test identifies healthy patients.
🔹 A highly sensitive test is useful for initial screening (e.g., periodontal probing).🔹 A highly specific test is important to confirm a diagnosis (e.g., advanced radiographs).
Would you rather miss a real case or falsely diagnose a healthy person?Understanding sensitivity and specificity helps you choose the right test for the right purpose! 🦷😊
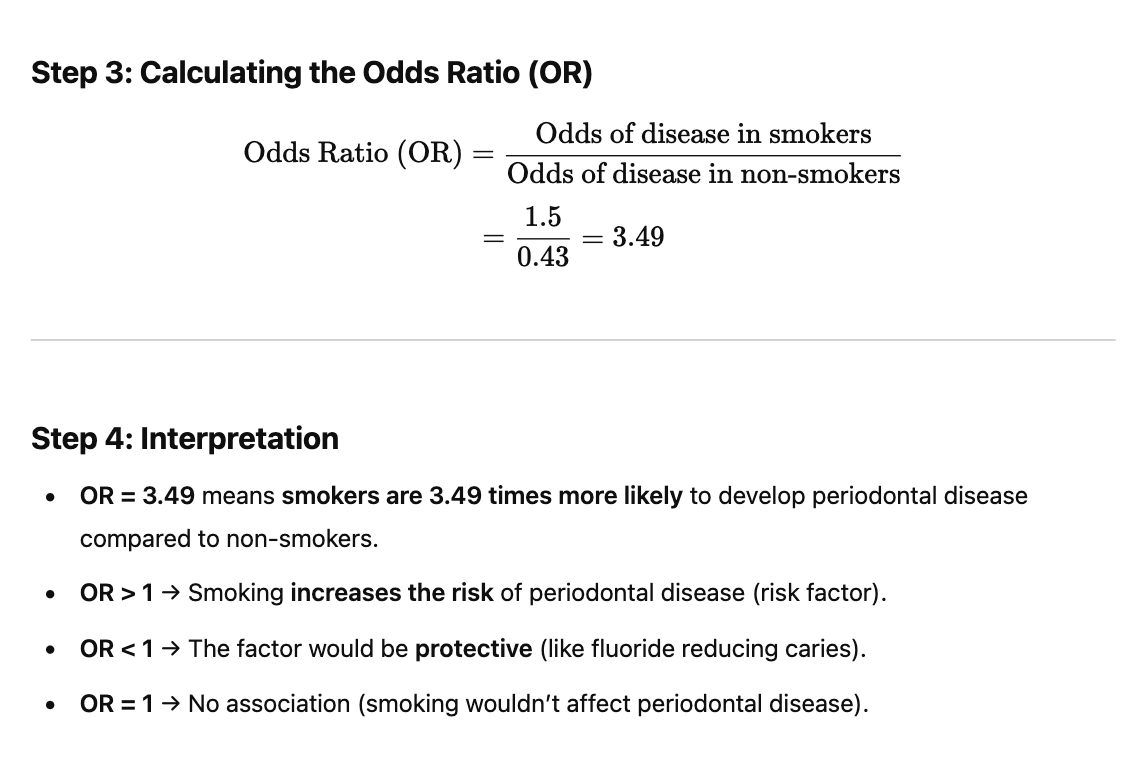
#Epidemiology 4- When the odds ratio is 0.3 and the 95% CI is (0.15-0.45) this indicates? ◯ A. There is strong evidence that the risk will lead to the event.◯B. There is weak evidence that the risk will lead to the event.◯ C. There is strong evidence that the risk will not lead to the event.◯ D. There is a weak evidence that the risk will not lead to the event.
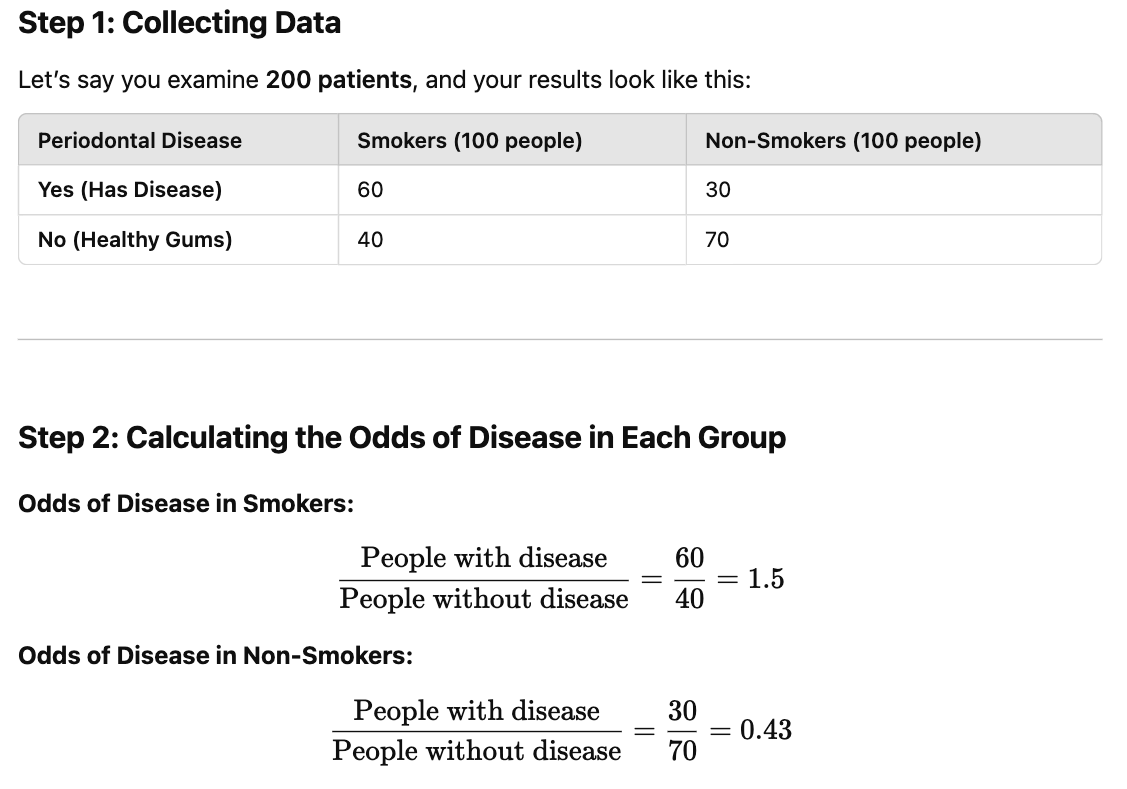
The Odds Ratio (OR) is a measure of association between an exposure (risk factor) and an outcome (disease/event).
Final Conclusion✔ Odds Ratio (0.3) suggests a strong protective effect.✔ The entire confidence interval (0.15-0.45) is below 1, meaning the risk is significantly lower.✔ There is strong evidence that the exposure reduces the event occurrence.
👉 Final Answer: (c) There is strong evidence that the risk will not lead to the event.
#Epidemiology5-A newly developed device designed for measuring oro-facial pain is under evaluation. The device provides consistent readings among the subjects, however, there is a lack of correlation between the device's readings and the subjects' self-reported pain index. Based on this information, which of the following best describes the performance of the device?
◯A. Low sensitivity and high specificity.◯ B. High sensitivity and low specificity.◯ C. High reliability and low validity.◯ D. Low reliability and high validity.
◯A. Low sensitivity and high specificity.
Understanding Reliability vs. Validity

Join our AFK Weekly newsletter
Solving questions is really important, but solving exam grade questions with true and authenticated answers is critical.
Will post a question everyday, then at the week end will do a video to explain the correct answers and the concept of each questions, signup now to get weekly updates.
Will post a question everyday, then at the week end will do a video to explain the correct answers and the concept of each questions, signup now to get weekly updates.
Thank you!